While you've been googling symptoms of hot flushes and irregular periods, something far more serious has been happening inside your body. Your bones – the framework that's supported you for decades – are quietly becoming more fragile. And the window to do something meaningful about it is narrower than anyone tells you.
This isn't about old ladies with walking frames. This is about you, right now, in your forties and fifties, when the decisions you make could determine whether you're hiking mountains at 70 or afraid to step off a curb.
The Hormone Highway Robbery
Oestrogen isn't just about reproduction – it's been your bones' bodyguard for years. This hormone actively promotes bone formation and slows down bone breakdown. When oestrogen levels start their perimenopausal rollercoaster, your bones lose their primary protector.
The statistics are stark: women can lose up to 20% of their bone density in the five to seven years following menopause. That's not a gradual decline – it's a precipitous drop that happens faster than you'd lose muscle mass from being bedridden.
"I had no idea," says Rachel, 47, from Leeds. "My mum broke her hip at 75, and I thought that was just old age. Nobody told me the damage was probably starting when she was my age."
The Invisible Timeline
Here's what's happening inside your body right now: bone tissue is constantly being broken down and rebuilt in a process called remodelling. Pre-menopause, this happens in careful balance. Post-menopause, the breakdown accelerates while the rebuilding slows down.
The cruel irony? You won't feel this happening. Bones don't ache as they weaken. There's no pain, no obvious symptoms, no warning signs. The first indication many women get is when they break something from what should have been a minor fall.
"I broke my wrist putting out the bins," recalls Jennifer, 58, from Southampton. "Slipped on wet leaves and put my hand out to break my fall. The doctor said my bones were like those of an 80-year-old. I was 52."
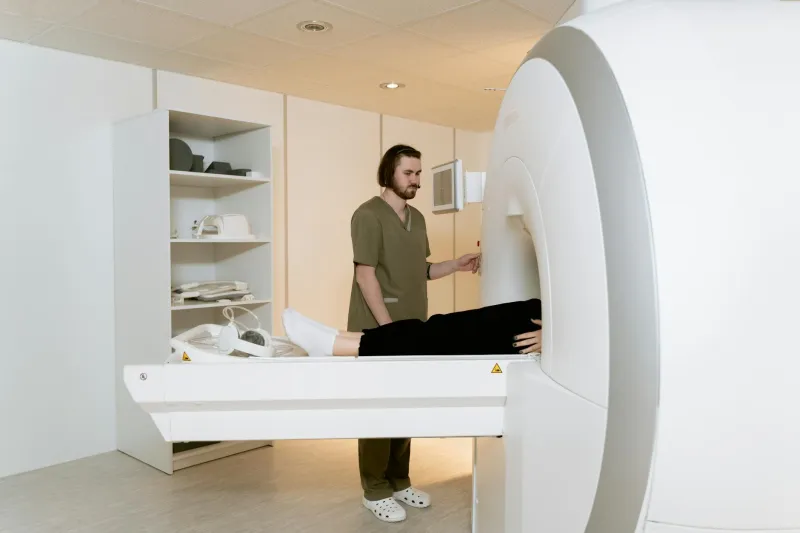
The DEXA Scan Lottery
A DEXA scan (Dual-Energy X-ray Absorptiometry) measures bone mineral density and can predict fracture risk. It's painless, quick, and incredibly informative. So why isn't every perimenopausal woman getting one?
The NHS criteria for DEXA scans are frustratingly narrow. You typically need to be over 65, have already broken a bone, or have specific risk factors like long-term steroid use or a family history of hip fractures.
"I asked my GP about a bone density scan when I started HRT," says Amanda, 49, from Birmingham. "She said I was too young and to ask again in 15 years. Fifteen years! By then, any damage would be done."
Private DEXA scans cost between £150-300 and might be the best money you spend on your health. Knowledge is power, and knowing your baseline bone density in your forties gives you actionable information rather than guesswork.
The HRT Question Nobody's Answering Clearly
Hormone Replacement Therapy (HRT) is the most effective treatment for preventing menopausal bone loss. Studies show it can reduce fracture risk by up to 30%. Yet the conversation around HRT often focuses on breast cancer risk while barely mentioning the bone protection benefits.
"My GP spent 20 minutes talking about blood clots and cancer risks," says Carol, 52, from Glasgow. "She mentioned bones in passing, like an afterthought. But when I looked at the research, preventing osteoporosis seemed like the strongest argument for HRT."
The timing matters crucially. Starting HRT during perimenopause or early menopause provides maximum bone protection. Starting it years later, after significant bone loss has occurred, is less effective.
The Supplement Confusion
Walk into any health shop and you'll be bombarded with calcium supplements promising stronger bones. The reality is more complex.
Calcium alone isn't enough – you need vitamin D to absorb it properly, and vitamin K2 to direct it to your bones rather than your arteries. But even the perfect supplement cocktail can't replicate what oestrogen does for bone health.
"I was taking calcium religiously," says Susan, 55, from Manchester. "Felt like I was being proactive. Then I found out my vitamin D levels were in the toilet, so I wasn't absorbing any of it properly."
The NHS recommends adults get 700mg of calcium daily from food sources, and 10 micrograms of vitamin D. But many women are deficient in vitamin D, particularly in the UK's limited sunshine.
The Exercise Prescription That Actually Works
Not all exercise is created equal when it comes to bone health. Gentle yoga and swimming, while excellent for other aspects of health, don't provide the mechanical stress bones need to stay strong.
Weight-bearing and resistance exercises are crucial. This means activities where your bones work against gravity: walking, dancing, tennis, weightlifting. The impact stimulates bone formation.
"I started lifting weights at 48," says Patricia, now 54, from Bristol. "Felt ridiculous at first, but my follow-up DEXA scan showed my bone density had actually improved. My trainer said I was stronger than some women 20 years younger."
The key is consistency and progression. Your bones need regular, ongoing stimulus to maintain and build density.
The Lifestyle Factors Nobody Mentions
Smoking accelerates bone loss. Excessive alcohol interferes with bone formation. Being significantly underweight removes the mechanical stress that keeps bones strong. These factors compound the hormonal changes of menopause.
Caffeine can interfere with calcium absorption if consumed in large quantities. Some medications, including certain antidepressants and proton pump inhibitors (for acid reflux), can affect bone density over time.
Taking Control of Your Bone Future
The first step is getting informed. Ask your GP about your personal risk factors. If you have a family history of osteoporosis, early menopause, or have taken certain medications, push for earlier screening.
Consider a private DEXA scan if NHS criteria don't apply to you but you want baseline information. Knowledge of your bone density can inform decisions about HRT, exercise, and lifestyle changes.
Get your vitamin D levels checked – this is available on the NHS if you have symptoms of deficiency, or privately for around £30.
The Conversation We Should Be Having
Bone health should be part of every menopause conversation, not an afterthought. The decisions you make in your forties and early fifties will determine your mobility and independence in your seventies and eighties.
"I wish someone had explained this 10 years ago," reflects Mary, 61, from Newcastle, who was diagnosed with osteoporosis after a vertebral fracture. "I thought menopause was about hot flushes and mood swings. I had no idea my skeleton was falling apart."
Your bones are worth fighting for. The time to act isn't when you're 65 and already osteoporotic – it's now, while you still have the power to protect and preserve them.
Don't let the silent steal continue. Your future self will thank you for paying attention to what's happening beneath the surface.